Healthcare is a complex and constantly evolving field, and with the increasing demand for quality and accessible care, new challenges arise. However, with these challenges come opportunities for innovation and the development of new healthcare solutions.
The Future is Now: Revolutionary Healthcare Innovations

Innovation In Healthcare
Healthcare innovation constantly pushes the boundaries of what is possible, resulting in improved health outcomes, better patient experiences, and increased efficiency in healthcare delivery. From the development of new medical technologies to the implementation of innovative approaches to care, healthcare innovation can revolutionize the industry and transform patients’ lives.
Healthcare Innovation: Addressing Challenges with Creative Solutions
The healthcare industry faces several significant challenges today. Here are some of the biggest challenges:
Rising Costs: Healthcare costs continue to escalate, straining individuals, families, and healthcare systems. Factors such as expensive medical treatments, technological advancements, and an aging population contribute to the rising costs.
Access to Care: Many individuals struggle to access quality healthcare services, especially in underserved communities or rural areas. Limited access to healthcare providers, long wait times, and inadequate health insurance coverage hinder receiving timely and affordable care.
Aging Population: The aging population presents unique challenges, such as increased demand for healthcare services, chronic disease management, and long-term care. Healthcare systems must adapt to meet the specialized needs of older adults and ensure quality care for this demographic.
Chronic Disease Management: Chronic diseases, such as diabetes, heart disease, and obesity, are on the rise and pose significant challenges for healthcare providers. Managing chronic conditions requires ongoing care coordination, patient education, and lifestyle modifications to prevent complications and improve overall health outcomes.
Healthcare Disparities: Disparities in healthcare access, quality, and outcomes persist among different populations, including racial and ethnic groups, low-income individuals, and marginalized communities. Addressing healthcare disparities is crucial for achieving equitable and inclusive healthcare for all.
Technological Advancements: While technology brings numerous benefits to healthcare, it also introduces challenges. Healthcare organizations must adapt to rapidly evolving digital technologies, ensure data privacy and security, and integrate technology effectively to enhance patient care and clinical workflows.
Workforce Shortages: Shortages of healthcare professionals, including physicians, nurses, and allied health workers, pose a significant challenge to healthcare systems. The demand for healthcare services exceeds the available workforce, leading to increased workloads, burnout, and compromised patient care.
Health Information Exchange: Seamless health information exchange between healthcare providers remains challenging. Fragmented health records and lack of interoperability hinder efficient communication, care coordination, and patient safety.
Healthcare technology is changing fast, but maybe not as quickly as we had hoped.
Healthcare Innovation: Solutions for Complex Health Challenges
| Healthcare Innovation | Description |
|---|---|
| Introduction | The healthcare industry constantly faces numerous challenges requiring innovative solutions, including rising costs, access barriers, and evolving patient needs. Exploring new approaches is crucial to effectively addressing these issues. This article delves into healthcare solutions and highlights innovative techniques transforming the industry. |
| Telemedicine and Virtual Care | Telemedicine and virtual care are powerful tools for expanding healthcare access and improving patient outcomes. They enable remote consultations, virtual visits, and remote monitoring, allowing timely medical attention without in-person visits. These technologies are vital in rural areas or during crises that limit physical access. |
| Wearable Technology and Remote Monitoring | Wearable devices like smartwatches and fitness trackers empower individuals to control their health. They monitor vital signs and activity, providing real-time feedback. Remote monitoring allows providers to monitor chronic conditions remotely, intervening when necessary, reducing readmissions, and improving outcomes. |
| Artificial Intelligence in Healthcare | Artificial Intelligence (AI) revolutionizes healthcare by enhancing diagnostic accuracy, predicting disease outcomes, and optimizing treatment plans. AI algorithms analyze vast patient data to identify patterns and provide valuable insights for healthcare professionals in areas like radiology, image recognition, and predictive analytics for disease management. |
| Precision Medicine | Precision medicine tailors medical treatments by considering an individual’s genetic makeup, lifestyle, and environment. Analyzing genetic data and leveraging advanced technologies allows personalized treatment plans, leading to more effective outcomes and minimized adverse reactions. |
| Blockchain in Healthcare | Blockchain technology offers secure and transparent data management in healthcare. It enables secure sharing of medical records, protects patient privacy, and efficiently manages healthcare transactions by eliminating intermediaries and enhancing data integrity. Thus, it could potentially revolutionize healthcare data management and streamlining processes. |
| Conclusion | Innovation is critical to addressing healthcare challenges. Embracing technologies like telemedicine, AI, wearable devices, precision medicine, and blockchain enhances patient care, improves outcomes, and optimizes healthcare delivery, paving the way for a more accessible, efficient, and patient-centric system. |
Tips for Implementing Healthcare Solutions
Implementing new healthcare solutions can be challenging, but some key strategies can help:
- Involve stakeholders: Engage healthcare providers, patients, and community members in developing and implementing new solutions.
- Start small: To test the effectiveness and feasibility of new solutions, begin with a pilot program or small-scale implementation.
- Monitor outcomes: Continuously monitor and evaluate the impact of new solutions to identify areas for improvement and ensure successful implementation.
- Seek funding: Find funding opportunities and partnerships to support developing and implementing new solutions.
Current situation and the future (Telemedicine Solutions)
Blood pressure measurement and mobile health diagnostics are practical and scalable for chronic disease detection and management. By maximizing the smartphone’s optics and computational power, they could assess physiological information from the morphology of pulse waves and thus estimate cuffless blood pressure (BP).
With its patented OptiBP technology, Biospectal provides accurate blood pressure measurements and management at the point of care—in less than 10 seconds.
High blood pressure (BP) remains the leading risk factor for death and disability in both high and low-income countries. Its complications are responsible for the deaths of approximately ten million people annually, a 50% increase over the estimates from 1990. By 2025, the number of people suffering from hypertension will reach 1.5 billion. The impact of this disease represents a daunting burden to any healthcare system.
Digital health approaches, particularly mobile health (mHealth) diagnostics, can be practical, scalable, and sustainable for chronic disease prevention and management. Mobile phones represent a widespread, readily available device for mHealth. Worldwide, over one-third of consumers own a mobile phone.
If the accuracy of reliable smartphone-based blood pressure measurements were to be demonstrated, this would be a promising tool that could improve access to more populations, medical record-keeping, analysis of blood pressure measurements for hypertension management, medication compliance, and health education.
How Biospectal OptiBP Works
The Biospectal OptiBP app runs on a typical smartphone and uses the built-in camera to record a user’s blood flow via their fingertip quickly and easily. A measurement is rendered in approximately 20 seconds, half the time of a typical blood pressure cuff.
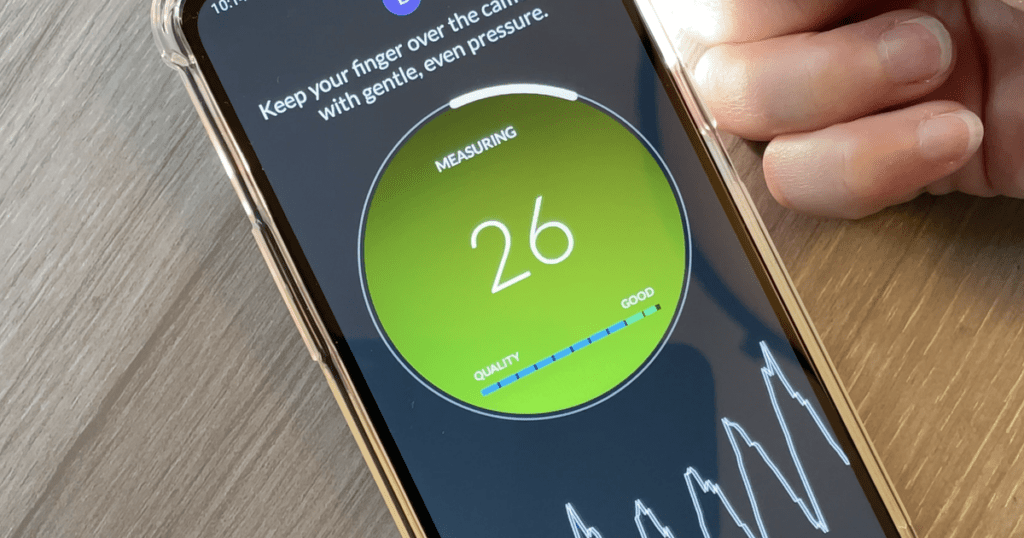
Biospectal’s proprietary algorithms and optical signal capture methods transform the captured data into blood pressure values. Additionally, the captured blood pressure data connects seamlessly with a user’s clinicians to support treatment regimens that help improve health, longevity, and quality of life.
Wearable Technologies benefits include:
- Connected remote patient monitoring shortens the pathway from measurement to action in a clinical regimen;
- Easy to use with an existing, ubiquitous device, the smartphone removes adherence barriers;
- Allows users to measure and monitor their blood pressure in their ‘natural’ environment, which is where blood pressure should be monitored;
- App form factor offers continuous product improvement and feature updates, and
- Unprecedented data insights drive higher value for drug development and lower insurance costs.
No other blood pressure monitoring and management device on the market offers both the medical-grade accuracy and convenience of Biospectal.

Healthcare innovations are constantly shaping the medical landscape, improving patient care, and transforming the healthcare industry as a whole
thank you for your comment on my post about healthcare innovations. I appreciate your interest in this topic. Healthcare innovations are indeed a fascinating and dynamic area, continually transforming the industry to improve patient care and outcomes.
Innovative tech is revolutionizing healthcare! From telemedicine to AI diagnostics, these advancements call for content that educates and engages both patients and practitioners.
Absolutely! These innovative healthcare solutions are paving the way for a healthier future. It’s inspiring to witness the power of technology and creative thinking in addressing the challenges we face. Let’s keep pushing for progress! #HealthTech #InnovativeHealthcare #HealthcareForward
Healthcare innovation is a rapidly evolving field that has the potential to transform the way we approach healthcare. I’m excited to see how the latest innovations in telemedicine, artificial intelligence, and machine learning are being used to improve patient outcomes and reduce healthcare costs
Exciting times ahead!
Adopting new technologies in healthcare facilities can significantly improve patient outcomes and operational efficiency. Yet, the integration of these technologies often requires overcoming substantial financial and training barriers, especially in under-resourced settings
Innovations in healthcare are truly shaping the future of medicine. It’s incredible to see how technology and new approaches are revolutionizing patient care and outcomes
The debate around healthcare innovation often revolves around challenges we face versus the potential for quick solutions.
Your article helped me a lot, is there any more related content? Thanks!